Understanding the Symptoms and Causes of an Esophageal Stricture
What is an Esophageal Stricture?
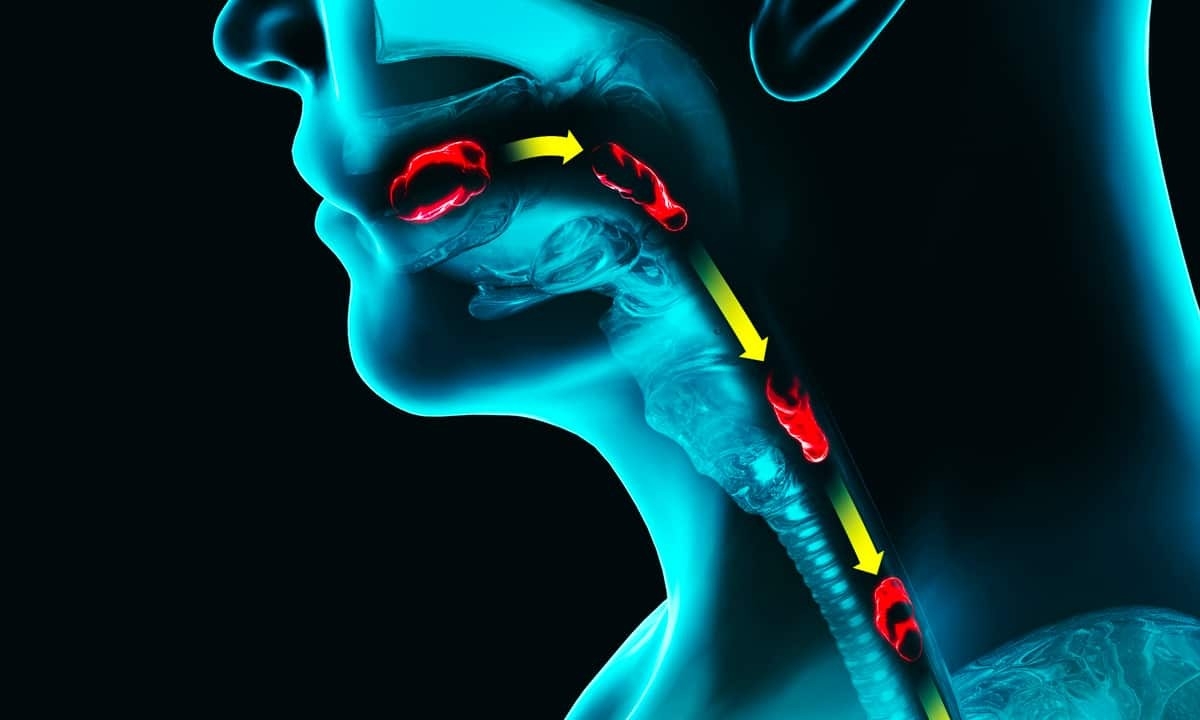
If you’ve ever had difficulty swallowing but didn’t know why, it might be because of an esophageal stricture. To understand how and why this happens, it’s helpful to first look at the function of the esophagus. The esophagus is the muscle-wrapped tube that extends from the mouth to the stomach and represents the first section of the digestive system. Under normal circumstances, food is chewed up and moistened in the mouth and is pushed down to the stomach by muscle contractions all along the esophagus.
There are times, however, when the esophagus becomes abnormally tightened or narrowed in a way that disrupts the normal digestive process. This abnormal narrowing is called an esophageal stricture, and for some people can be a very distressing condition. It is also sometimes referred to as a benign esophageal stricture (or peptic stricture), and that simply indicates that it isn’t cancerous. Anyone can develop an esophageal stricture, though it tends to be more common as people get older (especially over the age of 40).
Esophageal Stricture Symptoms
The primary symptom of this condition is dysphagia, the medical term for difficulty swallowing food or liquids. For many people, it can even feel like something is stuck in the throat or that food is moving down the esophagus at a greatly reduced rate. These sensations can also sometimes be felt more broadly in the back of the throat or across the upper abdomen. The severity of the symptoms tends to increase as the esophageal passageway gets narrower and narrower.
At first, the narrowing of the esophagus may not even be detectable to the patient. As the tightening continues, pills or small bits of solid food may be difficult to swallow. Eventually even liquids can become difficult to swallow. If left untreated, the difficulty swallowing can cause a person to actually eat and drink less and lead to dehydration or malnutrition. Additional symptoms may also include:
- heartburn
- pain when swallowing
- regurgitation
- unexpected weight loss
- drooling
- repeating episodes of choking
What Causes Esophageal Strictures?
There are a variety of possible causes behind the development of esophageal strictures, but the most common causes tend to involve diseases and disorders that cause inflammation and the subsequent formation of scar tissue (fibrosis). In some cases it can also be caused by neoplasia, the medical term for the abnormal growth of tissues; an incidence caused by neoplasia can then lead to malignancy and cancer. Below are examples of some of the most common causes:
- Gastroesophageal reflux disease (GERD): GERD, also known as chronic heartburn, is by far the most common cause of esophageal strictures. In patients with GERD, the ring of muscle that separates the stomach and esophagus (lower esophageal sphincter) does not function properly. As a result, stomach acid regularly makes its way up the esophagus and irritates the esophageal lining. Over time, inflammation and scar tissue can lead to a narrowing of the esophagus.
- Eosinophilic esophagitis: Though this condition isn’t well understood, it appears to be related to food allergies. White blood cells (not normally located in the esophagus) cause inflammation when exposed to a particular allergen; this inflammation can eventually cause scarring and narrowing in the esophagus.
- Radiation therapy: Oncologists sometimes prescribe radiation therapy for the treatment of certain types of cancer in the head or abdomen. In the process of eliminating cancerous cells, however, the radiation can also cause damage to the esophagus (and other parts of the body). This kind of damage from radiation often takes up to a year or longer after the therapy to manifest as esophageal strictures.
- Surgery: Any type of surgery performed on the esophagus has a chance of causing damage to the lining. Depending on the scale and severity of the damage, scar tissue can build up and thereby narrow the esophagus.
- Endoscopy: An endoscope is an amazing device that allows surgeons to examine the digestive system and perform surgery without the need for incisions. Yet sometimes an endoscopic procedure (or simply because of friction from movement) can cause damage to the esophageal lining. Just like with surgical damage, it can become fibrosed and tighten the passage.
- Infection: The immune response to various types of both viral and fungal infections causes inflammation on the inner lining of the esophagus. As with other sources of inflammation, strictures of the esophagus can form over time. There is also an increased risk factor for patients who are immunocompromised.
- Medication: There are numerous medications that have the potential to cause stricture-inducing inflammation or other effects that damage the esophagus. Two common examples are non-steroidal anti-inflammatory drugs (NSAIDs) and antibiotics. Prolonged use of these medications can gradually damage the esophagus.
- Ingestion of chemicals: Swallowing harmful chemical substances (accidental or otherwise) is unfortunately an all too common occurrence, especially among young children. In addition to other potential dangers, exposure of the esophagus to caustic substances can lead to esophageal strictures.
- Hiatal hernia: In a hiatal hernia, an abdominal organ has been abnormally pushed out through the muscles of the diaphragm. Since the site of the lower esophageal sphincter (LES) is where the diaphragm and stomach meet, a hernia in this area can sometimes cause the LES to malfunction. This can then lead to acid reflux and GERD.
Diagnosis and Treatment
Diagnosis of esophageal strictures will always begin with a standard physical examination and a review of the patient’s medical history. A precise diagnosis requires some specific tests that will verify the condition. One of the most common tests performed is an upper GI endoscopy; the doctor uses the camera on the endoscope to directly observe the lining of the esophagus to look for damage or scarring. If a stricture is confirmed, the endoscope can also be used to perform a biopsy so the tissue sample can be tested to rule out esophageal cancer.
If endoscopy isn’t an effective option for some reason, there are also other imaging tests that can be used to diagnose the condition. One example is an X-ray with a barium swallow. In this test, the patient swallows a solution containing barium; once the harmless barium spreads throughout the body, an X-ray can help highlight any abnormalities. The doctor may also use ultrasound or esophageal manometry for diagnostic purposes, depending on the patient’s circumstances.
If benign strictures are confirmed, the usual first treatment option is called esophageal dilation. In this procedure, the doctor will typically place a special dilating balloon (also known as a bougie) into the esophagus; when inflated, the balloon stretches out the esophagus and thereby eases symptoms like dysphagia. Depending on how complex and severe the strictures are, multiple esophageal dilation sessions may be necessary for sufficient relief. For some patients, symptoms may reoccur and require periodic dilation. Although minor, there is a risk of esophageal perforation with this procedure. Below are some additional treatment options that may be employed:
- Stents: Esophageal stents are usually reserved for malignant strictures, and the aim of stent placement is to hold the stricture open for a prolonged period of time. Eventually the tissue around the stent should remain the same size once the stent is removed.
- PPIs: Proton pump inhibitors are a class of medication that can reduce the production of stomach acid. They are also used to treat GERD and make damage to the esophagus less likely.
Contact Cary Gastroenterology
While benign esophageal strictures are rarely serious, it is a condition that requires medical intervention. At Cary Gastro, we are passionate about providing excellent digestive healthcare and the quickest path to improving quality of life. If you have been experiencing any of the symptoms noted above, please contact us to request an appointment.